Degenerative disc disease, a common cause of chronic back pain, can make it painful to sit on a beach chair, swing a golf club, or even bike along the boardwalk. In a city known for wellness and fitness, such pain isn’t just a minor inconvenience – it’s a barrier to fully enjoying the healthy, active life Miami Beach residents value. In fact, disc-related back pain (also called discogenic pain) is one of the leading reasons people seek medical care, and it’s a top cause of disability worldwide. Active individuals often find themselves caught between wanting relief and avoiding solutions that might sideline them further. This is where regenerative therapies like Platelet-Rich Plasma (PRP) are stepping in as game-changers, offering hope of natural healing without major surgery or long-term medication
Understanding Degenerative Disc Disease (DDD)
Degenerative disc disease isn’t truly a “disease” at all – it refers to the wear-and-tear changes in the spinal discs that can lead to pain. Spinal discs are the rubbery, cushion-like pads between each vertebra in your spine, acting as shock absorbers and allowing flexibility. Over time, these discs undergo natural aging and stress-related changes. They gradually dry out and flatten, losing the water content that provides cushioning. Tiny cracks or tears can form in the tough outer layer of a disc from repetitive strain or injury. When that outer wall weakens, the disc’s soft center can bulge or even herniate (slip out), potentially irritating nearby nerves.
Multiple factors contribute to DDD. Age is the biggest risk factor – nearly everyone’s discs show some degeneration by age 60, though not everyone has pain. However, active lifestyles and injuries can accelerate the process. Years of sports, lifting weights, running, or even just lifting a heavy suitcase the wrong way can add up to more disc stress. Past back injuries, even minor ones, can hasten degeneration down the line. There’s also a genetic component – if your parents had disc problems, you might be predisposed. Other factors like smoking (which impairs disc nutrition) and obesity (which adds spinal load) further increase risk.

What does degenerative disc pain feel like? Often, it’s a dull or sharp pain in the lower back that worsens when sitting and bending and feels better when you change positions or lie down. Long drives or sitting at your desk can become agonizing, while a short walk or gentle yoga provides relief. Many with DDD report stiffness and “flare-ups” of back pain after strenuous activity. If a degenerated disc bulges and presses on a nerve root, it can cause sciatic pain – that radiating pain, numbness, or tingling that travels from the buttock down the leg (sciatica). In fact, lumbar disc herniation due to degeneration is one of the most common causes of sciatica in active adults. Lumbar degenerative disc disease tends to strike in the lower spine (L4-L5, L5-S1 levels), which is why it’s a frequent culprit in lower back pain and sciatica cases. The condition typically surfaces in middle age (40s – 50s), but even younger people can experience disc problems – especially athletes and physically active individuals who’ve put a lot of mileage on their backs.
Dealing with degenerative disc pain can be frustrating. It’s chronic in nature – meaning it persists or recurs over months and years – yet it often responds only partially to rest or pain pills. Many Miami Beach residents who pride themselves on staying fit are faced with an unpleasant choice: avoid the activities they love or suffer through the pain. Fortunately, medical science is offering a promising third option: healing the discs and relieving pain through the body’s own regenerative power – namely, Platelet-Rich Plasma therapy.
What Is Platelet-Rich Plasma (PRP) Therapy?
Platelet-Rich Plasma therapy is an innovative treatment that taps into your body’s natural healing abilities. PRP is made from your own blood. A small sample of blood is drawn and then spun in a centrifuge to concentrate the platelets – cell fragments that are rich in growth factors and healing proteins. The result is a golden-colored plasma with a platelet concentration far above normal. When this concentrated PRP is injected into an injured area (like a degenerated disc), it delivers a powerful dose of growth factors that stimulate tissue repair and reduce inflammation. In essence, PRP acts as a natural booster shot for your body’s healing process.
Originally popularized in sports medicine for tendon and ligament injuries, PRP therapy has gained traction across many musculoskeletal conditions. Health-conscious patients appreciate that it’s autologous – meaning it comes from their own body, with no foreign drugs or synthetic chemicals involved. For an affluent wellness-focused community, PRP holds appeal as a treatment aligning with a “heal-from-within” philosophy. That said, PRP is also evidence-based: research has shown PRP can help regenerate tissues by:
- Stimulating cell growth and migration: At the injection site, PRP’s growth factors signal cells to multiply and move in to repair damage.
- Increasing collagen and extracellular matrix production: This can strengthen and rebuild tissues like disc cartilage, which needs collagen for structure.
- Modulating inflammation: Rather than simply blocking inflammation (as steroids do), PRP tends to normalize the inflammatory process, potentially leading to more effective healing.
In the context of lower back pain, PRP therapy can be applied in a few ways. For facet joint arthritis (another common back pain source), PRP can be injected into the joints. For soft tissue issues like strained ligaments or muscles, PRP can be injected into those tissues. But one of the most exciting uses – and the focus of this article – is intradiscal PRP therapy, where PRP is injected directly into a degenerated spinal disc to treat discogenic back pain.
Intradiscal PRP Therapy: How It Works for Spinal Discs
Intradiscal PRP therapy is a specialized application of platelet-rich plasma aimed at healing damaged spinal discs. If you’ve been told you have degenerative disc disease or a mild herniated disc that’s causing your chronic back pain, intradiscal PRP is designed for you. The concept is straightforward: by delivering growth factors right into a disc that has little blood supply of its own, we attempt to spark a repair process that the body couldn’t achieve on its own. Spinal discs normally receive very limited blood flow, which is why they don’t heal well after injury. PRP effectively overcomes the blood supply issue by bringing a concentrated dose of healing nutrients directly to the problem area.
During an intradiscal PRP treatment, the physician injects the PRP solution into the center of the affected disc, typically under X-ray or CT guidance for accuracy. Once inside the disc, the platelets release growth factors that can potentially encourage the disc cells to repair torn fibers and restore disc matrix. This may help the disc regain some height or at least slow further degeneration, and importantly, reduce the pain signals coming from that disc. Patients with discogenic pain often have fissures (cracks) in the disc’s outer layer and inflammation around spinal nerves; PRP’s anti-inflammatory and tissue-regenerative actions target both issues – helping seal up annular tears and calming the inflammatory chemicals that trigger pain.
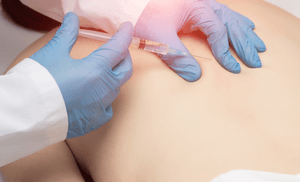
Overall, intradiscal PRP therapy represents a promising, natural repair strategy for disc-based back pain. By treating the root cause – a weak, degenerating disc – it aims to provide more lasting relief rather than the temporary fix one might get from a painkiller. And for active individuals, the allure is clear: heal the disc, so you can get back to your sport or daily routine without pain.
PRP vs. Traditional Spinal Injections: How Do They Compare?
When it comes to nonsurgical treatment for back pain, corticosteroid injections have been the conventional option for decades. If you’ve ever had an epidural steroid injection for sciatica or a facet joint steroid shot for arthritis, you know they can provide relief – but often it’s short-lived. Let’s compare traditional spinal injections (steroids) with PRP injections:
- Mechanism: Steroid injections are potent anti-inflammatories. They work by shutting down inflammation around irritated nerves or inside joints. This can provide quick pain relief, but it doesn’t fix underlying tissue damage. In contrast, PRP injections modulate inflammation and actively stimulate healing. PRP’s growth factors tackle the degenerative process itself by repairing tissues and fostering a healthier environment in the disc or joint.
- Duration of Relief: Steroids often bring relief for a few weeks or months. Unfortunately, the benefit may fade by around 3 months or sooner in many cases. Repeated epidural steroid shots for disc herniation show diminishing returns – the first injection might help a lot, the second less, and so on. PRP tends to have a slower onset (it might take a few weeks to notice improvement), but the relief builds over time and can last much longer as healing progresses.
- Side Effects and Risks: Cortisone (steroid) injections, especially if repeated, carry systemic risks – they can spike blood sugar in diabetics, temporarily raise blood pressure, and over time may contribute to bone density loss or weaken soft tissues. Locally, too many steroid shots can potentially hasten cartilage wear. PRP, on the other hand, is derived from your own blood with no additives; it’s generally very safe. The main side effect is temporary soreness or an inflammatory reaction as your body’s healing kicks in. Infection is an extremely rare risk for any injection, which applies to both steroid and PRP. Overall, PRP’s safety profile is excellent, making it attractive for those wary of steroid downsides.
- Goal of Treatment: We might say steroids are a “quick fix” – useful to calm a severe pain flare or enable you to participate in rehab by reducing pain. PRP is more of a “long game” – aiming to actually improve the condition of the disc or tissues. An insightful guideline by pain specialists notes that PRP is emerging as an important option between standard conservative care and surgery. If you’ve had some relief from steroid injections but don’t want to keep getting them, PRP could be the next step to try for a potentially longer-lasting solution.
Evidence is mounting that for discogenic back pain and sciatica, PRP can match or exceed the pain relief of steroids by 6 months, without exposing patients to steroid-related side effects. For a health-conscious individual, the idea of using your body’s own healing agents – instead of synthetic steroids – to treat back pain is highly appealing.

Who Is an Ideal Candidate for PRP (and Who Might Not Benefit)?
Ideal candidates for intradiscal PRP therapy are typically those with chronic lower back pain stemming from disc problems, who are looking for relief beyond what physical therapy and standard treatments have provided. You might be an excellent candidate if:
- You have confirmed discogenic pain: Perhaps an MRI showed degenerative discs or a mild disc bulge at the levels corresponding to your pain, and your doctor has determined the disc itself is likely the pain generator.
- Conservative treatments haven’t been enough: You’ve tried things like rest, physical therapy, chiropractic care, or mild pain medications and still have significant pain after months. Many PRP candidates have pain persisting at least 3 – 6 months despite these efforts.
- You want to avoid surgery or prolonged medication use: PRP appeals to those who don’t want to jump into spinal surgery (such as fusion or disc replacement) or rely indefinitely on painkillers, muscle relaxers, or repeat steroid injections. It’s a middle road – more proactive than just masking pain with pills, but far less invasive than surgery.
- Your condition is moderate (not severely advanced): The best results with PRP tend to be in mild-to-moderate degenerative disc disease – for example, a disc that’s thinning but not completely collapsed, perhaps with small herniations or tears. Research suggests patients with at least 50% of normal disc height and only small disc protrusions (≤5 mm) respond better. In other words, if you still have some disc tissue left to heal, PRP can likely help stimulate repair. Patients who had one or two-level disc issues seem to do better than those with more diffuse multi-level degeneration.
- You’re generally healthy: Since PRP is derived from your blood, your overall health matters. Ideal candidates can safely have their blood drawn and don’t have uncontrolled conditions that might impede healing. Being a non-smoker (or willing to stop smoking) is important, as smoking can slow recovery. Also, those not on blood thinners or who can pause them are preferred, because anti-clotting medications might reduce PRP’s efficacy.
On the other hand, PRP may not be suitable or as effective for:
- Severe spinal conditions requiring surgery: If you have major spinal instability, a large disc herniation compressing nerves severely, or symptoms like significant muscle weakness or loss of bowel/bladder control (red flags for surgical intervention), PRP is not appropriate. These cases often need surgical decompression or stabilization. PRP is a regenerative boost, not an urgent fix for emergency neurological issues.
- End-stage degeneration: If your disc has no height left (bone-on-bone) or you have advanced spinal arthritis with bone spurs compressing nerves at multiple levels, PRP injections alone might not provide dramatic relief. In such cases, structural changes may be too pronounced for PRP to overcome, and surgery might be the only reliable option.
- Patients with certain medical issues: Those with bleeding disorders or who can’t stop blood-thinning meds may be advised against PRP due to risk of bleeding. Active infections or cancer are also typically contra-indications for PRP in any area. Additionally, if you have a low platelet count or certain immune conditions, PRP preparation might be less effective.
- Someone expecting an instant cure: It’s worth noting that PRP is not a “quick-fix” miracle. Patients who aren’t prepared to invest in the recovery process (which can take weeks of patience) may be disappointed. Ideal candidates understand that PRP’s healing is gradual and are willing to follow post-procedure guidelines to maximize their outcome.
In a personalized consultation, a regenerative medicine specialist will review your MRI and history to determine if intradiscal PRP makes sense for you. For many active mid-life adults with stubborn back pain, the answer is increasingly yes – PRP is an option to finally mend the disc itself, not just mask the pain.
The PRP Treatment Process: Step by Step
When you decide to proceed with PRP therapy for your lower back, what exactly happens? The process at a regenerative spine clinic is straightforward and usually completed within a couple of hours. Here’s a step-by-step look at how a typical intradiscal PRP treatment is carried out:
The PRP procedure typically involves a thorough initial consultation, a blood draw to prepare the PRP, a precisely guided injection into the affected disc, and post-procedure recovery guidance. This streamlined process is usually completed in under an hour, start to finish.
- Personal Consultation: First, you’ll meet with the STEMS Health specialist (often an interventional orthopedic or pain management physician) for a detailed evaluation. They will review your medical history, perform a physical exam, and look at any imaging (like MRI) to pinpoint the degenerated disc causing your pain. This is when you’ll discuss the plan and ensure you’re a good candidate for intradiscal PRP. All your questions are addressed so you go in with realistic expectations and a clear understanding of the procedure.
- Blood Draw and PRP Preparation: On the procedure day, a nurse or phlebotomist will draw a sample of your blood – typically around 15 – 60 mL (which is a few tablespoons, similar to a routine lab test). The blood sample is immediately placed in a centrifuge machine, which spins it at high speed for about 10-15 minutes to separate out the components. This process concentrates the platelets into a smaller volume of plasma. The end product is Platelet-Rich Plasma, ready for use. It’s worth noting that everything is done following strict sterile techniques; PRP is prepared in a closed sterile system to avoid any contamination.
- Image-Guided PRP Injection: The most critical step is the injection of PRP into your target disc. You’ll be positioned either on your stomach or side on a procedure table. The doctor will use imaging guidance – usually fluoroscopy (a live X-ray) for discs – to accurately guide a special thin needle into the disc space that needs treatment. (Sometimes, local anesthetic is used on the skin to minimize discomfort, and light sedation can be offered if you’re very anxious, though many people do fine with minimal sedation.) Once the needle is confirmed to be in the correct disc (they often use a tiny amount of contrast dye to verify placement under X-ray), the physician slowly injects the PRP solution into the disc. You might feel pressure or mild pain during the injection, as the disc expands slightly – this is normal and usually well-tolerated since it’s a small volume. The injection itself is over in just a minute or two. By delivering the PRP directly into the injured disc, this treatment kick-starts a localized healing reaction that will unfold over the coming weeks.
- Post-Procedure Observation: After the injection, you will rest in the clinic for a short period (perhaps 15-30 minutes) while the staff monitors you. Unlike surgery, there’s no need for a prolonged recovery room stay – most patients walk out on their own shortly after, since only local anesthesia is used. You might feel that your back is a bit sore or stiff from the injection – again, this is expected. Before you leave, you’ll be given specific aftercare instructions.
- Recovery Guidance and Follow-Up: The medical team will go over do’s and don’ts for the days following PRP. Typically, you’re advised to take it easy for the first day or two – go home, rest, and avoid intense activities. However, complete bed rest is not recommended; gentle movement is encouraged even the next day (short walks, simple stretching) to keep blood flowing. Very importantly, you will be told not to take anti-inflammatory medications (like ibuprofen or naproxen) for several weeks. The reason is that inflammation is a key part of the healing process that PRP initiates; taking a high-dose NSAID could blunt the very effect we want. You also should avoid using ice or heat on your back for the first 72 hours, and skip the hot tubs or saunas for a few days – basically, let your body do its thing without interference. The doctor might recommend wearing a lumbar brace for a short time or give guidance on safe stretching. Many clinics suggest starting physical therapy or supervised exercises within a week or two post-injection, focusing on core stabilization and gentle mobility (specific timing can vary, with some preferring PT start at 4 – 6 days post-PRP and others waiting a few weeks). You’ll also schedule a follow-up appointment so the doctor can check your progress, often at 4-6 weeks after the injection.
This step-by-step process is usually completed in under an hour of procedure time, plus some prep and post-observation. There’s no general anesthesia, no incisions, and you’ll go home the same day. For a busy professional or an active parent in Miami, that means minimal disruption to your schedule. Nonetheless, what happens after the procedure – the recovery phase – is just as important for a successful outcome, so let’s paint a picture of what you can expect in the days and weeks following your PRP disc injection.
Recovery Timeline and Tips After PRP Treatment
Healing after an intradiscal PRP injection is a gradual journey, and knowing what to expect can help you navigate it with confidence. Here’s a general recovery timeline and some tips for each stage:
- Immediate Aftermath (Day 0-1): On the day of the injection, you’ll likely feel some soreness or achy pain in the lower back. Don’t be alarmed – this post-injection soreness is common and actually a sign that the PRP’s inflammatory healing response is kicking in. When you get home, take it easy. You can do light walking around the house, but avoid any strenuous activity or lifting. It’s fine to lie down in a comfortable position – many patients ask about sleeping after PRP, and generally you can sleep however you feel most comfortable. If lying flat hurts, try elevating your legs with a pillow or lying on your side with a pillow between your knees. Avoid taking NSAID pain relievers (no Advil, Motrin, etc.); if you need pain control, use acetaminophen (Tylenol) or a pain medication prescribed by your doctor that doesn’t interfere with inflammation. Also, skip any ice or heat on your back for the first 3 days, as extreme temperatures can interfere with the intended inflammatory process. Gentle breathing exercises or mindfulness can help with discomfort on Day 1. Many patients are able to return to office-type work the next day if needed, provided it’s not physically demanding.
- Early Recovery (First Week): Through days 1-3, expect some ups and downs in back soreness. You might feel a bit stiff getting up in the morning. By the end of the first week, acute soreness from the injection usually improves. During this week, light movement is your friend. Short, frequent walks (even 5-10 minutes around the block) help stimulate blood flow without over-stressing the healing disc. Avoid heavy lifting, intense workouts, or prolonged bending/twisting. You might start some gentle stretches or physical therapy exercises as instructed – often things like pelvic tilts, gentle lumbar range-of-motion movements, or core activation exercises. The goal of Week 1 is to remain mobile enough that you don’t get deconditioned, but calm enough that your disc can start its repair work. Some patients also report feeling a flare of their typical back pain or leg pain during this week – this can happen as the PRP induced inflammation is present. As long as it’s tolerable, don’t panic; it should be transient.
- Weeks 2-4: Building Strength and Seeing Improvement: By the second and third week after PRP, many patients notice that the initial post-injection discomfort has subsided. You may even start to sense early improvements – perhaps the back pain isn’t as constant or the sciatica episodes are less intense. Clinical studies have noted significant pain reduction often becoming measurable around the 4-week mark. During weeks 2-4, you will typically ramp up a more structured rehabilitation program. Under guidance from a physical therapist or your doctor’s advice, you can introduce stretching routines, core strengthening exercises (like modified planks or Pilates-based moves), and low-impact cardio (stationary biking, swimming, or brisk walking). It’s still key to avoid heavy lifting or high-impact activities. This period is crucial for supporting the regeneration: you want to engage muscles to support your spine (promoting good biomechanics) without overloading the healing disc. Listen to your body – mild soreness after exercise is okay, sharp pain is not. By week 4, many people have noticeable improvements in daily function: sitting for longer is easier, morning stiffness is less, and reliance on pain medication drops.
- Weeks 4-8: Gradual Return to Activity: Around the one to two-month mark, you’ll likely have a follow-up with your provider to evaluate your progress. If all is going well, you’ll continue advancing your activity levels. During weeks 4-6, patients often start to reintroduce more of their normal lifestyle – perhaps swinging a golf club in practice, doing light jogs, or a gentle yoga class – with their provider’s okay. By 6-8 weeks, if your pain has significantly decreased, you may be cleared for even more activities. Keep in mind, healing is still ongoing. One study noted that patients continued to improve between 2 months and 6 months after intradiscal PRP. So, don’t rush into maxing out your workouts even if you feel great at two months. Gradual progression is key. If you’re a tennis player, you might start with half-speed swings; if you’re a gym-goer, maybe return to weight machines before heavy free weights. The core strength and stability you’ve built in therapy will help protect your back as you ramp up.
- Beyond 2 Months (3-6+ Months Out): This is where, for many, the real payoff of PRP is evident. By 3 months, a lot of patients report significant pain reduction – some on par with how they felt before their disc became a problem. Daily activities and even sports can often be done with little or manageable pain. At 6 months, the improvements tend to stabilize, and studies show sustained benefits at this point. If PRP has successfully helped regenerate or repair your disc, the relief can be long-lasting. It’s not unusual for patients to continue to be pain-free or greatly improved at 1 year post-treatment. During this phase, you’ll likely be back to full activities, including rigorous exercise, if all has healed well. Your doctor might obtain a follow-up MRI around 6-12 months to see structural changes, though clinical improvement is the main goal. It’s important to maintain a healthy lifestyle to protect your spine – regular exercise, strong core muscles, good posture habits, and perhaps occasional “maintenance” check-ins with a physical therapist or chiropractor can all help prolong your back health.
Throughout the recovery, communication with your provider is important. If something doesn’t feel right or pain worsens significantly at any point, you should inform them. Occasionally, some people might require a second PRP injection months later if progress plateaus, but many get what they need from just one treatment. Patience is key – regenerative therapy is not an overnight fix, but rather a progressive improvement. The reward for that patience, however, can be getting back to the Miami Beach lifestyle you love, without the chronic pain that used to hold you back.
Why Miami Beach Patients Are Choosing PRP for Back Pain Relief
In Miami Beach’s wellness-driven community, it’s no surprise that more patients with back pain are electing PRP therapy over surgery or long-term medication. Several compelling reasons are behind this trend:
- Natural, Evidence-Based Healing: Today’s patients are savvy – they want treatments that not only work, but also align with a natural approach to health. PRP checks both boxes. It uses your body’s own platelets to heal tissue, and it’s supported by a growing body of clinical evidence for conditions like degenerative disc disease and sciatica. Rather than relying on opioids (with their risk of addiction) or cortisone injections (with temporary effect), people see PRP as a way to fundamentally improve their condition. Miami Beach residents who invest in organic food, yoga, and high-end fitness also appreciate that PRP is an organic solution – it’s literally part of you – harnessed in a high-tech way to fix a problem.
- Minimal Downtime, Maximum Gain: Unlike surgery, which might have you in a brace and off the tennis courts for months, PRP therapy entails minimal downtime. After a single outpatient injection and a few days of taking it easy, you’re already on your way, slowly increasing activity. By a few weeks out, most people are back to the bulk of their daily routines, just avoiding extreme exertion early on. Compare that to a lumbar fusion surgery, which could mean weeks of post-op pain, substantial rehab, and possibly limited mobility for a long period. PRP offers a much quicker return to daily life, which busy professionals and active retirees alike find very appealing. As one local clinic notes, intradiscal PRP is a non-surgical alternative with minimal recovery time, allowing patients to get back to daily activities more quickly.
- Avoiding the Risks of Surgery and Chronic Meds: Every intervention has risks, but surgery (even minimally invasive) carries significant considerations – anesthesia, infection risk, potential complications like nerve injury, and the possibility that surgery might not fully relieve the pain or could create new issues (such as adjacent segment problems after fusion, or scar tissue). Many Miami Beach patients with disc issues aren’t keen to roll those dice unless absolutely necessary. PRP, being so low-risk, is an attractive first-line before considering the knife. Similarly, relying on long-term medication is unattractive to the health-conscious – who wants to take pain pills or muscle relaxers forever? PRP offers a chance at lasting relief that reduces or eliminates the need for daily meds. And since PRP can be repeated or combined with other regenerative therapies (like stem cell treatments) if needed, patients feel they have a continuum of options before surgery enters the picture.
- Active Lifestyle and High Performance: PRP is aligned with maintaining that lifestyle – it’s about improving function. Patients who undergo PRP often do so because they want to continue playing sports or exercising, not just lie in bed without pain. By healing the disc and strengthening the back, PRP aims to enable people to resume high-level activities. We’ve seen that by 3-6 months post-PRP, many individuals are back to playing tennis or swinging a golf club without the old pain flaring up. In contrast, a spinal surgery might make one wary of returning to impact sports, or long-term steroid use might weaken tissues and actually make activities riskier. PRP can actually make the tissue more robust by stimulating repair. For a community that runs on the motto of “work hard, play hard,” PRP fits perfectly – fix the issue and get back in the game.
In essence, Miami Beach patients are choosing PRP because it aligns with their values – health, activity, and longevity. They are leveraging advanced medical science to heal in a way that feels authentic and sustainable. PRP empowers patients to take control of their recovery, using their own biology to combat pain, rather than surrendering to invasive procedures or a lifetime of pill bottles. For many, it’s a worthwhile investment in restoring the pain-free, active life that defines living in this vibrant coastal city.
Chronic lower back pain from degenerative disc disease can be a stubborn foe, especially for those of us unwilling to give up our active lifestyles. But as we’ve explored, Platelet-Rich Plasma therapy offers a compelling path forward. By healing the disc from within, PRP addresses back pain at its source – all while allowing you to avoid major surgery and minimize ongoing reliance on medications. PRP therapy represents the perfect marriage of cutting-edge medical innovation and natural, evidence-based healing.
If you’re tired of living life on the sidelines due to lower back pain, it may be time to consider intradiscal PRP therapy. Imagine months from now, feeling stronger and waking up without that familiar ache – and knowing you achieved it with a treatment that worked with your body, not against it. Many patients in our community have already made this choice and are back to hiking, swimming, and dancing through life with a renewed appreciation for pain-free movement.
Don’t let back pain define your Miami Beach lifestyle. Talk to a STEMS Health spine specialist about whether PRP could be the solution for you. We will evaluate your condition and guide you through the process with the expertise and personal care befitting an individualized therapy. You deserve a life free from chronic pain – and with PRP therapy’s help, that vibrant, active life you envision may be well within reach.