Why you should ensure your doctor is using ultrasound or fluoroscopy when treating certain areas with stem cells, exosomes, or PRP.
Why should you make sure your doctor is using ultrasound or fluoroscopy during your regenerative medicine treatments?
Regenerative medicine, a rapidly evolving field that harnesses the body’s innate healing capabilities, has witnessed remarkable advancements in recent years. At the forefront of these cutting-edge therapies are stem cell treatments, PRP treatments, and exosome treatments, which hold immense potential for tissue regeneration, repair, and functional restoration. However, the success of these treatments for many applications hinges on precise delivery and accurate targeting of the therapeutic agents to the intended sites within the body. This is where the crucial roles of advanced imaging such as ultrasound and fluoroscopy come into play, providing invaluable guidance and visualization during the administration process. These advanced imaging techniques have become indispensable tools in the application of stem cell and exosome therapies, ensuring optimal outcomes and maximizing the potential for regeneration and healing.
Here are a few main reasons you should ensure your doctor is using ultrasound or fluoroscopy when treating certain areas with stem cells, exosomes, or PRP:
-
Proper assessment of tissue health and suitability
-
Real-time monitoring of the procedure
-
Precision in targeting specific areas for treatment delivery
-
Minimized complications & increased safety
1. Proper Assessment of Tissue Health and Suitability
Prior to treatment, ultrasound helps assess the condition of the affected tissues, offering valuable insights into the severity of degeneration, inflammation, or injury. This information is crucial in planning the treatment, identifying optimal injection sites, and determining the likelihood of a successful response.
This is especially important for patients with complex injuries: these imaging methods help verify the location and extent of damage, guiding clinicians toward the most appropriate treatment strategy.
2. Real-Time Monitoring of Procedures:
Both fluoroscopy and ultrasound provide immediate feedback, allowing the practitioner to monitor the placement of the needle in real-time and adjust it as needed. This immediate feedback ensures that the procedure is performed correctly and adjustments can be made on the spot if necessary.
3. Precision in Targeting Specific Tissues for Treatment Delivery:
Using ultrasound or fluoroscopy guidance allows clinicians to visualize the exact injection site, ensuring the treatments are delivered to the target tissue with high accuracy. Before and during the procedure, these techniques can assess the extent of damage and verify the correct treatment area, which is vital for tailored therapy approaches. This increases the likelihood of successful therapy by maximizing the regenerative impact at the damaged or injured area, and by minimizing the risk of misplacement that could lead to suboptimal outcomes or complications.
4. Minimized Complications & Increased Safety
By guiding the exact placement of needles or catheters, these imaging modalities reduce the need for multiple attempts, thus decreasing patient discomfort and potential tissue damage. This is especially important if the target area is near critical structures like nerves or blood vessels, and helps to reduce the risk of injury
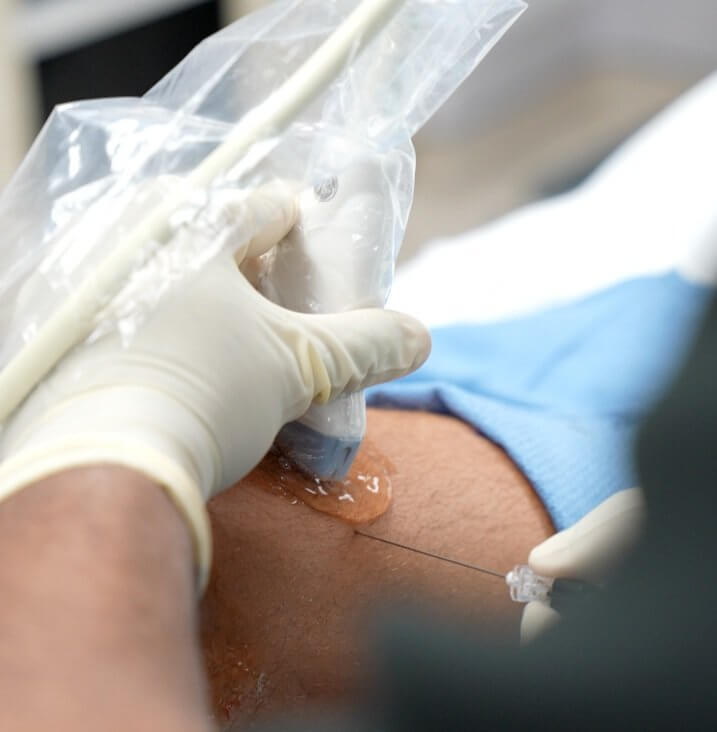
Dr. Choxi using ultrasound during a stem cell treatment of the knee
At STEMS, we always use either fluoroscopy or ultrasound when injecting these treatments in delicate areas of the body, such as the spine, knees, and other joints. These imaging methods provide a level of precision and safety that enhances the overall effectiveness of stem cell, PRP, and exosome treatments. While not always mandatory (many clinics don’t use these), we believe these methods are indispensable tools that help reduce complications and enhance efficacy.